Trésor-Economics No. 247 - Combating France's medical deserts
The "My Health 2022" plan proposes responses to the problem of medical deserts: the overhaul of health studies, the deployment of 400 general practitioners in under-dense areas, 1,000 territorial professional health communities, and the introduction of medical assistants. Other measures could reinforce the fight against medical deserts: encouraging people to settle in under-dense areas, adapting studies to boarding schools, raising the awareness of interns to internships in under-dense areas.
Since the 2000s, certain under-served regions of France known as "medical deserts" have had varying degrees of difficulty (depending on the medical specialty) in maintaining a sufficient supply of physicians. This situation persists despite the rollout of incentives – the effectiveness of which has yet to be assessed – for physicians to set up practice in under-served areas.
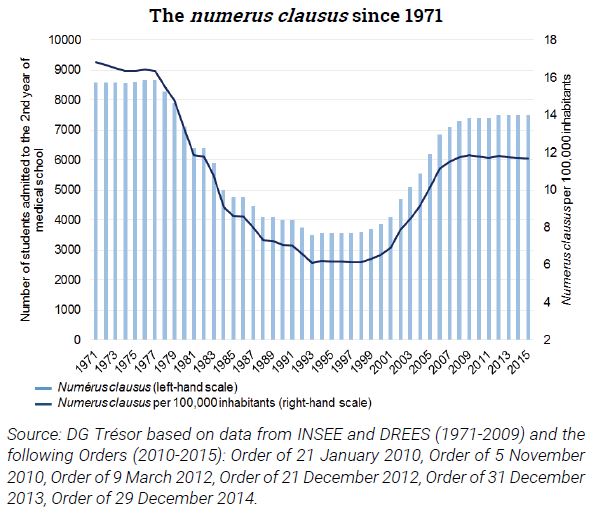
The "My Health 2022" plan includes long-term measures to address the shortage of physicians, which were enshrined in the Healthcare System Organisation and Transformation Act. These included eliminating the numerus clausus policy, which restricted the number of physicians at the end of the first year of medical school, and increasing the number of consultations per physician by creating the profession of medical assistant. However, supplementary solutions to regional imbalances could well prove useful, since an increase in the number of doctors may not itself improve the match between supply and demand for the benefit of under-served areas.
Without questioning the principle of freedom of establishment, a temporary, short-term adaptation of the principle could be considered in certain particularly over-served areas. This would help prevent a glut of supply where it is already quite high and improve matching between medical density and physicians' initial practice settlement. This could only be implemented gradually and in close consultation with physicians, to prevent a negative impact on the appeal of private practice
In addition, some measures could be taken during medical school:
– Directing medical residency positions towards setting up practices in these areas or making additional positions available for the first students redirected during the first cycle, provided they settle in an under-served area.
– Reallocating medical residency in attractive medical specialties to regions that have difficulty attracting new medical residents.
– Raising awareness amongst medical students about general practice in under-served areas.